Article
[Science Update] Relationship between metabolites modulated by HMOs and reduced risk of LRTIs
Public health
3 min read
Intervention
- Control formula: Intact cow’s milk protein-based formula
- Test formula: Control formula supplemented with 2 HMOs (2’-FL & LNnT) in which 1.5 g/L lactose was replaced by a 2:1 mixture of the 2 HMOs
Methods
- Shotgun metagenomic sequencing
- Untargeted mass spectrometry metabolomics
Results
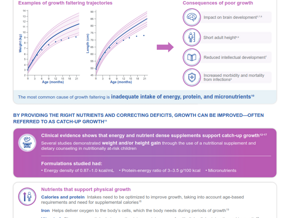
- Major alterations in lipid and amino acid metabolism were caused by the presence of HMOs in the formula, particularly in phospholipid/sphingomyelin metabolism and the gamma-glutamylation and N-acetylation of amino acids
- HMOs caused alterations in the gut's functional ecology, which were associated to the reduced LRTIs that have been reported
- A negative correlation between gamma-glutamylated amino acids (GGAAs) and LRTIs was observed
- Sphingolipids and free amino acids were observed to be positively correlated to later LRTIs
- There were several statistically significant correlations between the LRTI phenotype or feeding group and the three identified classes of important metabolites, namely GGAAs, N-acetylated-amino acids (NAAs), and sphingolipids
- Sphinganine and 3-keto-sphinganine had the strongest correlations with Bacteroides species
- GGAAs had the strongest correlation with Bifidobacterium species, namely, B. bifidum, B. longum subsp. longum, and B. longum subsp. infantis
- The concentrations in stool calprotectin and elastase and the stool metabolites sphinganine, 3-keto-sphinganine, 5-aminovalerate, butyrate, and propionate were observed to be positively correlated
- Stool calprotectin and elastase were observed to be negatively associated with the stool metabolites acetate, lactate, fucosyl-glycans and most GGAAs
Conclusion
- These results expand our knowledge of the infant gut/microbiome co-metabolism in early life and give evidence that such metabolic alterations may affect immune competence at distant mucosal sites like the airways
Abbreviations:
2’-FL = 2’-Fucosyllactose; LNnT = Lacto-N-Neotetraose
Link to the full article:
https://pubmed.ncbi.nlm.nih.gov/35990340/
Reference:
Martin FP et al. Host-microbial co-metabolites modulated by human milk oligosaccharides relate to reduced risk of respiratory tract infections. Front Nutr. 2022;9:935711.
Other articles that you might be interested in:
[Literature library] Human milk oligosaccharides and infant gut microbiota
WYE-EM-107-AUG-22
If you liked this post you may also like